Affinitē Benefit Query Engine (BQE)
Affinitē Benefit Query Engine™ (BQE)
Reimagine Utilization Management with Real-Time Benefit Intelligence
Empower smarter, real-time decisions with the first-of-its-kind Affinitē Benefit Query Module.
20K+
companies running through the BQE, the only solution of its kind in the market
35%
reduction in authorization volume reaching nurse or physician review
75%
reduction in authorization processing time
10x
faster in determining detailed benefit coverage, leading to more accurate claims payment
Health plans today face growing complexity in managing benefit variations, authorizations, and regulatory requirements. The Affinitē UM Dynamic Benefit Query Module, powered by our first-of-its-kind Benefit Query Engine™ (BQE), transforms this process through intelligent automation and real-time insights – reducing friction for users and providers alike.
Affinitē UM’s Benefit Query Engine is a breakthrough, AI-powered rules engine that redefines how authorizations are managed. It intelligently identifies, triages, and routes requests in real time – adapting to benefit design and clinical complexity with unmatched precision.
The result? Seamless process adherence, lightning-fast efficiency, and smart auto-approvals that set a new standard for utilization management.
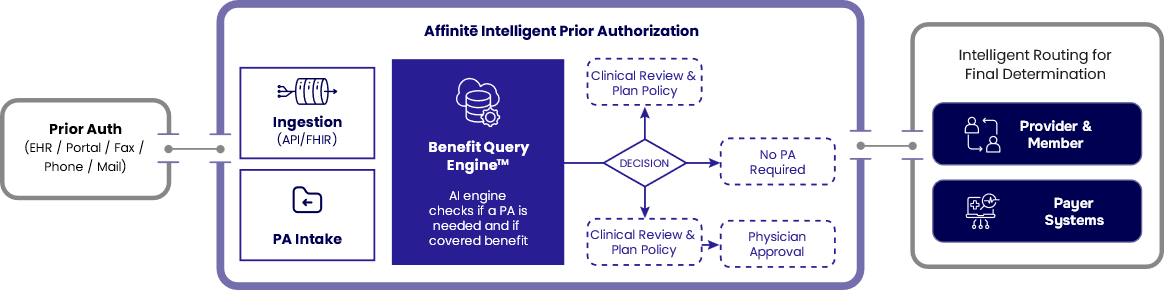
Built for UM and Medical Management Teams
Real-Time
Benefit Clarity
The Benefit Query Module embeds real-time benefits information directly into utilization management workflows. Once configured, it automatically alerts users when an authorization request should be handled differently – such as identifying benefit exclusions or services that do not require prior authorization.
Automated Decisions &
Provider Notifications
Through configurable rules, Affinitē UM can automatically approve or deny services based on client-defined criteria, instantly sending notifications to providers via outbound fax or 278 transactions. The result: fewer manual steps, faster decisions, and consistent compliance across every request.
Flexible, Future-Ready Architecture
The Benefit Query Engine™ (BQE) can be easily configured with a plan’s benefits data or integrated with an existing API for seamless information exchange. This flexibility ensures that health plans maintain control while modernizing their UM operations.
Case Study:
How a National Health Plan Transformed Utilization Management
A large national health plan faced significant operational challenges in its Utilization Management (UM) processes due to fragmented systems, siloed and manual workflows, and limited integration. To address these critical issues, the health plan partnered with Vital Data Technology (VDT) to implement the Affinitē Intelligent Prior Authorization (IPA) platform and transform their organizational utilization management processes. This case study examines the transformation journey, highlighting how VDT's innovative solutions addressed the plan’s complex operational challenges.
Complete the form to receive the full case study
Transforming the User Experience
By eliminating manual benefit lookups, the Benefit Query Module delivers immediate time savings and accuracy for front-line UM teams.
