growth in daily completed authorizations from 2023 to 2025.
22
drop in percentage of faxes due to switch to web/portal transmission
99 %
growth in Medicare Advantage daily authorizations completed
46
Streamline prior authorization workflows, cut costs, and elevate member care with intelligent, AI-driven automation.
Affinitē Utilization Management (UM) redefines utilization management through AI-driven intelligent automation and advanced analytics that power real-time, data-driven decisions. Our innovative Benefit Query Engine delivers instant visibility into eligibility and benefits, enabling proactive and precise determinations for every authorization.
Built for the future of healthcare, the platform adapts to evolving regulatory demands with configurable, intelligent tools that enhance oversight and transparency. By connecting providers, members, and care teams through a unified digital ecosystem, Affinitē UM transforms utilization management into a predictive, collaborative process – driving smarter decisions and better outcomes across the continuum of care.
Intuitive design and smart configuration for maximum productivity.
Intelligent rules engine
dramatically streamlines
UM processes.
360-degree visibility
and compliance across
all lines of business.
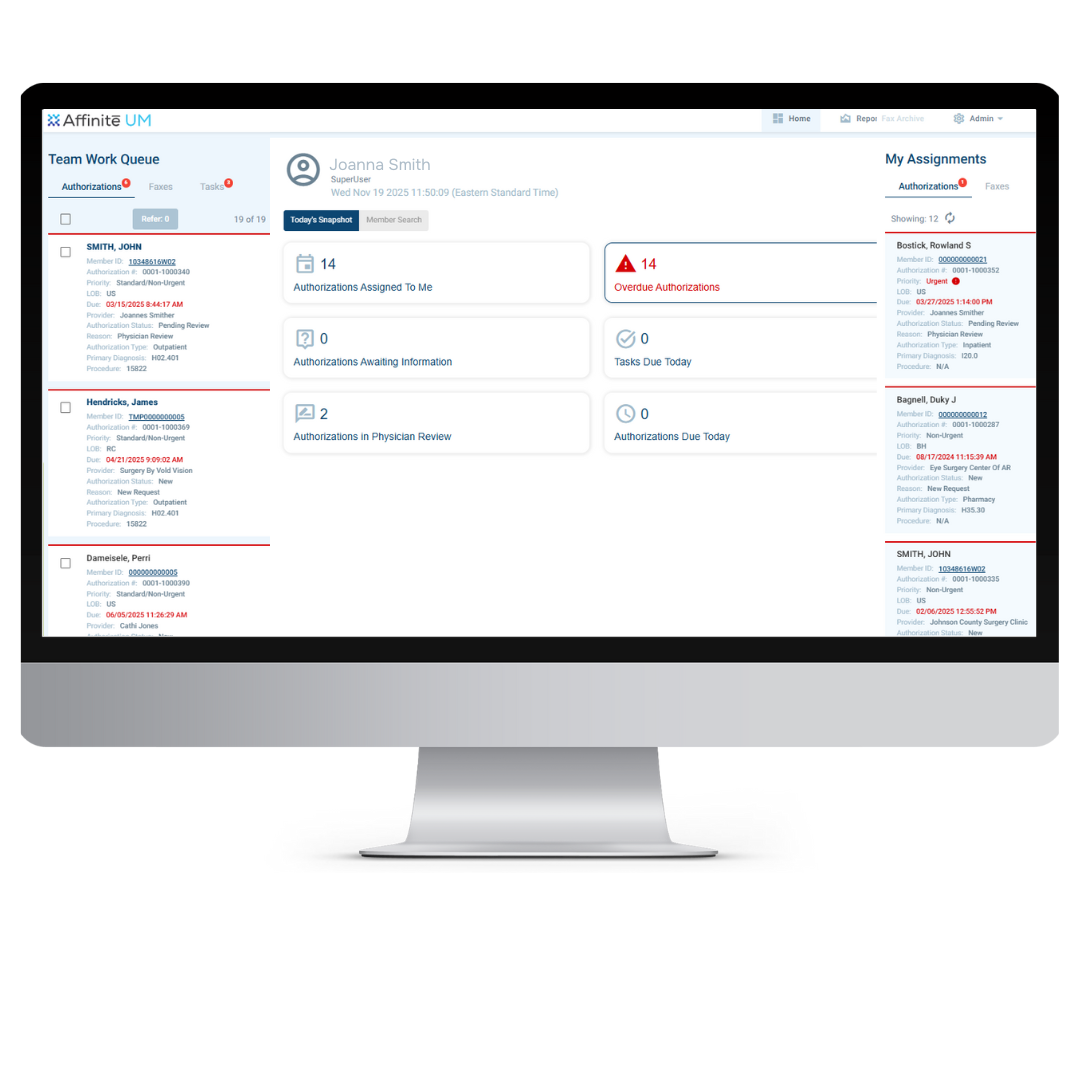
Designed specifically for health payers, Affinitē UM simplifies workflows, automates complex benefit verifications, and eliminates time-consuming administrative tasks. This frees valuable clinical staff to target only those complex cases that require their expertise. Intelligent automation streamlines administrative actions so your team can operate at the top of their licensure.
One-click referrals reduce review times from over an hour to less than 15 minutes.
Our user-friendly design streamlines authorization management by up to 40%.
Instant insights into member benefits; track statewide
compliance in real-time.
Our user-friendly design streamlines authorization management by up to 40%, saving significant time and money.
Plan-specific accommodations, turnaround time compliance, benefit configuration, and auto auth rules.
All authorization-related data is housed in one platform to sync care management, care gap, and other clinical systems.
Affinitē UM’s Benefit Query Engine is a breakthrough, AI-powered rules engine that redefines how authorizations are managed. It intelligently identifies, triages, and routes requests in real time – adapting to benefit design and clinical complexity with unmatched precision. The result? Seamless process adherence, lightning-fast efficiency, and smart auto-approvals that set a new standard for utilization management.

Affinitē UM is your trusted partner in navigating the upcoming CMS-0057-F mandates, effective January 1, 2027. With our cutting-edge platform, your team can confidently stay ahead of regulatory requirements, simplifying compliance while unlocking new opportunities for success.
Designed for precision and efficiency, Affinitē UM streamlines complex processes, ensuring your organization isn’t just compliant but thrives in an evolving regulatory landscape.
Payers are working to overhaul prior authorization, according to a recent announcement from AHIP. Discover how Vital Data Technology is leading the effort with advanced, intelligent solutions.
In this guide, we review actionable steps health plans should take to position themselves for the future state of prior authorization.
Discover how CMS's push for uniform prior authorization policies and automation can improve efficiency, increase member satisfaction, and reduce administrative burdens for health plans.