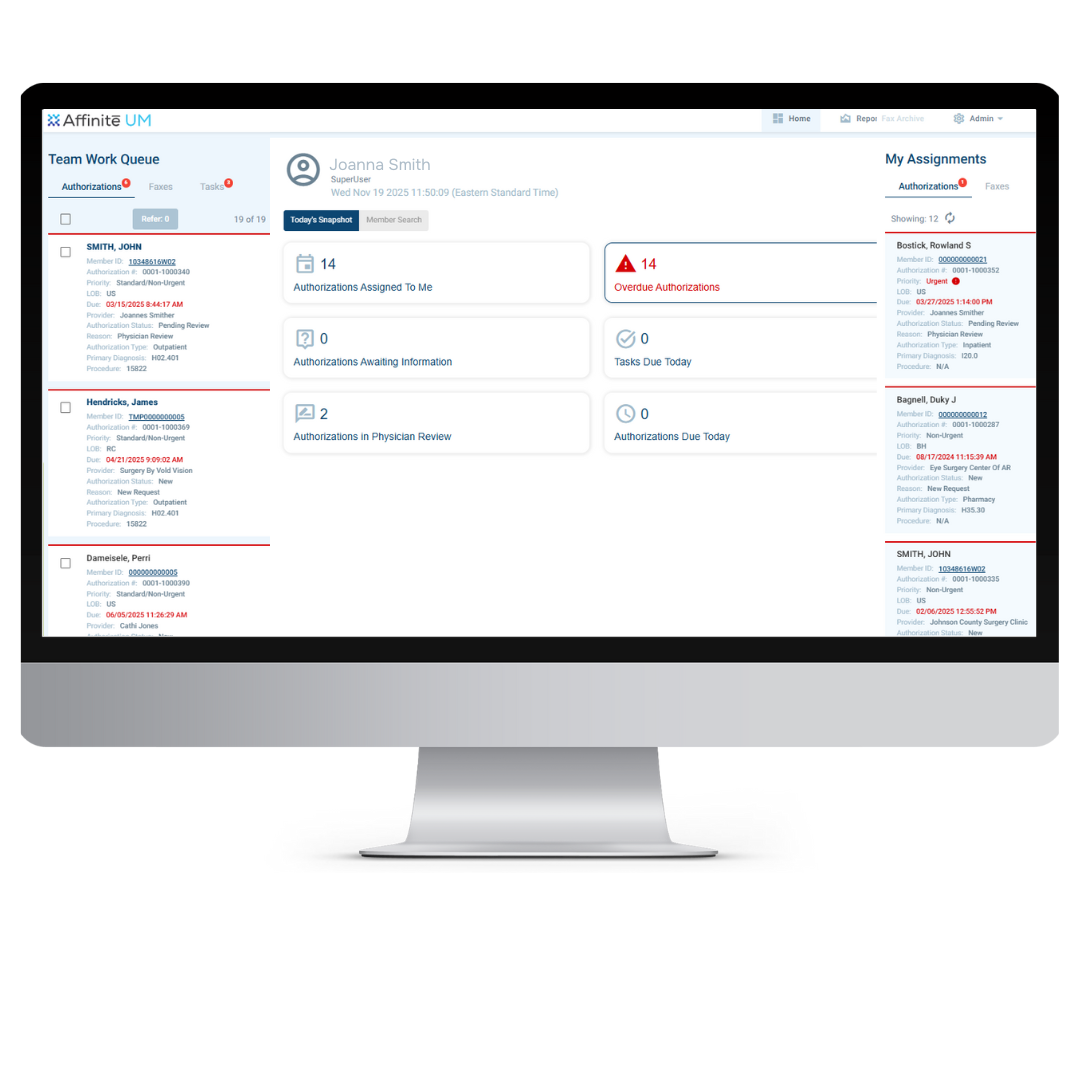
growth in daily completed authorizations from 2023 to 2025.
22
drop in percentage of faxes due to switch to web/portal transmission
99
%
growth in Medicare Advantage daily authorizations completed
46